Service
- Taking “voice of the customer” training, which advocates direct input from clients to improve a process or service
- Shadowing nurses to better understand their perspective and identify the root causes of complaints about late or missing medication
- Starting the morning shift 30 minutes earlier to ensure timely delivery of medications
What can your team do to listen to the voice of your customers? Especially if those customers are fellow employees in a different department?
Format:
PDF
Size:
8.5"x11"
Intended audience:
Frontline employees, managers and teams
Best used:
Use this tool to learn about the Southern California Attendance Program Standard.
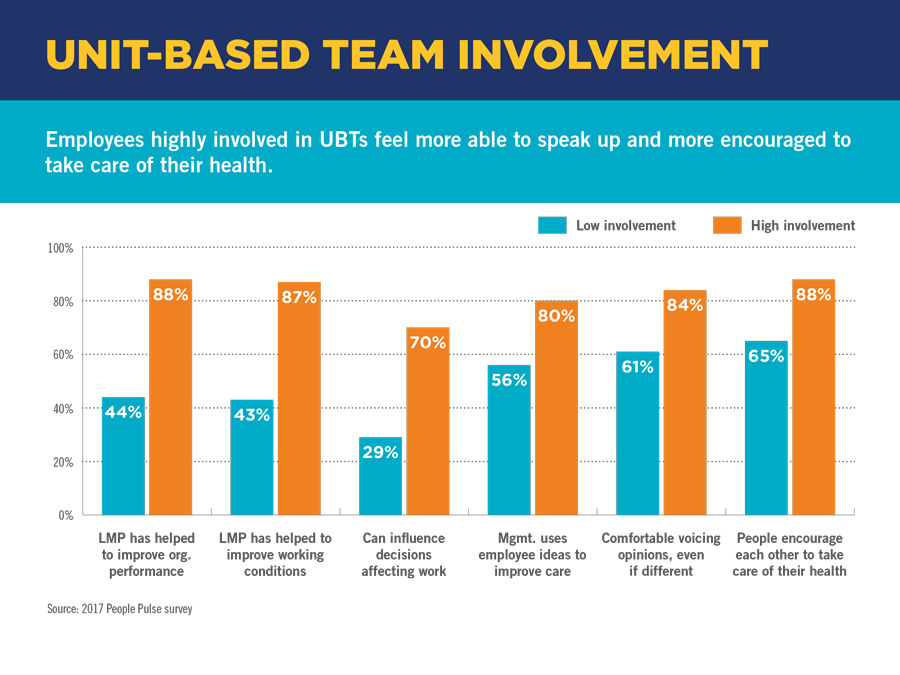
Fewer injuries, higher patient satisfaction, more influence over decisions: Good things happen when people get involved in their unit-based team. See the People Pulse survey findings.
Do teams get better results when frontline workers are engaged, free to speak and can influence decisions? Yes, say the people who know best — Kaiser Permanente workers and managers themselves.
Recent People Pulse surveys confirm that unit-based teams get positive results for health plan members and patients, the organization and workers themselves.
For instance, the 2017 People Pulse survey of more than 155,000 KP employees showed that when union-represented employees are highly involved in UBT activities, they get 29 percent higher scores on measures of their willingness to speak up — a key driver of patient and workplace safety and satisfaction. They also get 33 percent higher scores on questions regarding workplace health and wellness.
Improved safety and satisfaction
Further analysis, included in the 2016 People Pulse survey, showed that teams with high employee involvement have:
- 18 percent fewer workplace injuries
- 13 percent fewer lost work days
- 4 percent higher patient satisfaction
“Our findings show that employees who are highly involved in their unit-based teams feel more able to speak up and more encouraged to take care of their health,” says Nicole VanderHorst, principal research consultant with KP Engagement & Inclusion Analytics. “That makes them more likely to have better performance outcomes.”
A better way to work
Workers’ greater propensity to speak up and look after their health when they’re involved in team activities covers several questions (see chart below). For example, workers who are highly involved in their UBTs are far more likely to say:
- The Labor Management Partnership has helped improve organizational performance and working conditions.
- They can influence decisions affecting their work.
- They’re comfortable voicing differing opinions.
- Management uses their ideas to improve care.
- They’re encouraged, and encourage others, to take care of their health.
Roots of workforce engagement
All these factors contribute to a better employee experience as well as performance. And UBTs reflect KP’s unique history with the labor movement.
“Henry Kaiser was perhaps the 20th century’s most worker-friendly industrialist. He supported organized labor and knew that people step up when allowed to exert their job experience, as they do with UBTs,” says KP archivist and historian Lincoln Cushing. “He trusted employees to make decisions that benefitted themselves and their organizations.”
If you belong to a unit-based team — and most union-represented employees do — talk with a team co-lead about ways to get more involved.
Tips for Reducing Wait Times
Show our members you know their time is valuable. Try out these tips for reducing wait time and improving efficiency.
Tips for Improving the New Member Experience
When we help KP membership grow, we help make KP strong and our jobs more secure. One of the best ways to do that is to create a "wow" experience for new members.
Tips for Improving Attendance
When our employees show up, they are at the ready to provide the best care and service to our patients and members. These tips will help you tackle attendance problems to keep your team running smoothly.
Once a patient is discharged from the hospital and returns home, the burden of care often falls to family and friends. But how do we care for the caregivers? A new initiative looks for answers.
Beep! Beep! Beep! The electronic sound of Cary Brown’s alarm clock wakes him at 5 a.m.
The Kaiser Permanente member rises to shower and make breakfast, careful not to disturb his sleeping wife, Elissa, who is recovering at home after surgery on a broken leg at the Woodland Hills Medical Center in Southern California.
On top of completing household chores, the retired Hollywood TV director spends his day making sure Elissa is comfortable and pain-free.
The experience has taken a toll on him.
“The hours of staying awake and the repetitive nature of it—and not having any life at all outside of home—is very difficult,” says Brown, who worked on the hit TV series Doogie Howser, M.D.
Now he’s part of an ambitious effort by the Southern California region to enhance support for caregivers, who play a vital role helping to heal and comfort patients outside the hospital. By reducing caregivers’ social isolation, integrating them into the hospital care team and addressing their health needs, regional leaders hope to improve patient safety and quality in the home.
‘Human-centered design’
Under the initiative, frontline workers, physicians and managers are partnering with KP members and their families to design the ideal in-home care experience for patients and caregivers. Participants are using a creative approach to problem solving known as human-centered design, which starts with the people you’re designing for and ends with solutions that are customized to their needs.
“It’s a way to engage the folks who are most affected from day one,” said Dr. Nirav Shah, senior vice president and chief operating officer for Clinical Operations in Southern California. “No program that I could ever design will be as good as one that had the people who are most affected design it with us. It’s about empathy and understanding.”
Human-centered design is also an ideal tool for unit-based teams to use on performance improvement projects. It delivers on the fundamental concept of the Value Compass—to put the member and patient at the center of decision making—and both frontline workers and Labor Management Partnership leaders, from management and the Coalition of Kaiser Permanente Unions, have been supporting the caregiver project.
Reducing the overwhelm factor
At a meeting in Pasadena, the participants—patients and caregivers, KP employees and physicians—gathered in small groups to share personal tales and draw storyboards to help identify barriers, come up with potential solutions and provide insights to regional Home Health leaders.
Shawna Wallace, a senior physical therapist for Home Health and member of UNAC/UHCP, said the experience was eye-opening.
“I’ve gone into homes where caregivers really care about their loved ones, and they are extremely overwhelmed,” she said. “This is a great opportunity for us to see where we can make better programs for our caregivers and members in these scenarios.”
Brown is hopeful that the approach will give caregivers—and their loved ones—the emotional and physical support they need to thrive.
“If you take care of the family as a unit,” Brown says, “you make it possible for each individual in the family to be better.”
Listening Is Key for Audiology Co-Leads
How a shared appreciation of each other’s different skills and background helps this unit-based team succeed.
The Road Taken
Key accomplishments in workforce planning and development, workplace safety, total health, joint marketing and growth and attendance (and a peek into the future).